How to Identify Death Stages, Estimate Time of Death, and Interpret What You See at Necropsy
Introduction
When a veterinarian arrives to examine a dead animal — whether in a field, a barn, or a clinic — one of the first and most critical tasks is not to immediately perform a necropsy, but to read the body. The postmortem (PM) changes already underway carry a wealth of information: how long the animal has been dead, what position it died in, whether it was moved, and how decomposed the tissues will be when you open the carcass.
Misinterpreting postmortem artefacts as antemortem lesions — or missing genuine pathological findings buried within decomposition changes — is one of the most common errors in veterinary pathology. This guide walks through every stage and type of postmortem change, explaining the underlying biology, practical timelines, and what each finding means for your examination and death-time estimation.
Part 1: The Three Categories of Postmortem Change
Postmortem changes are conventionally grouped into three temporal phases:
Immediate changes occur at the moment of death and represent somatic (systemic) death — the irreversible cessation of brain, heart, and lung function.
Early changes develop over the first hours to days. These include the classic signs used to estimate time of death: algor mortis, rigor mortis, and livor mortis, along with cadaver dehydration, postmortem emphysema, and imbibition.
Late changes encompass decomposition, putrefaction, mummification, and skeletonization — the progressive biological breakdown of all organic tissues.
Understanding which phase the carcass is in before you begin your necropsy is essential for accurate interpretation.
Part 2: Immediate Changes — The Signs of Death
What Happens at the Moment of Death
Immediate postmortem changes reflect somatic death — the simultaneous and irreversible failure of the three vital systems:
- Brain: Permanent cessation of neurological function
- Heart: Complete failure of circulatory function
- Lungs: Entire and permanent cessation of respiration
These manifest clinically as:
- Loss of consciousness and insensibility
- Loss of voluntary muscle movement
- Cessation of breathing
- Cessation of heartbeat and pulse
- Absence of reflexes (corneal, pupillary, pedal)
During this period, primary muscle relaxation occurs — the body becomes completely flaccid immediately after death, before rigor mortis sets in. This brief window of relaxation is an important early sign that the animal has only recently died.
Practical Tip: On first approach to a carcass, check for responsiveness, corneal reflex, mucous membrane color, and muscle tone before touching or repositioning the body.
Part 3: Early Postmortem Changes
1. Cadaver Dehydration
One of the very first visible changes after death is desiccation of exposed mucous membranes and skin. With circulation stopped, the body’s tissues begin losing moisture through evaporation.
What you will observe:
- Ocular, buccal, and genital mucous membranes become dry and opaque
- Skin takes on a darker color than normal tissue
- Corneal opacity develops as the eyeball retracts (sinks) and the cornea loses transparency
- The previously moist, glistening surfaces of mucous membranes become dull
Factors influencing the rate of dehydration:
- High environmental temperature → faster drying
- Low humidity and good ventilation → faster drying
- Dense coat/wool → slows surface evaporation
Forensic significance: Sunken, opaque eyes combined with dry mucous membranes indicate that death occurred at least several hours prior to examination, though exact timing depends heavily on environmental conditions.
2. Algor Mortis — Cooling of the Body
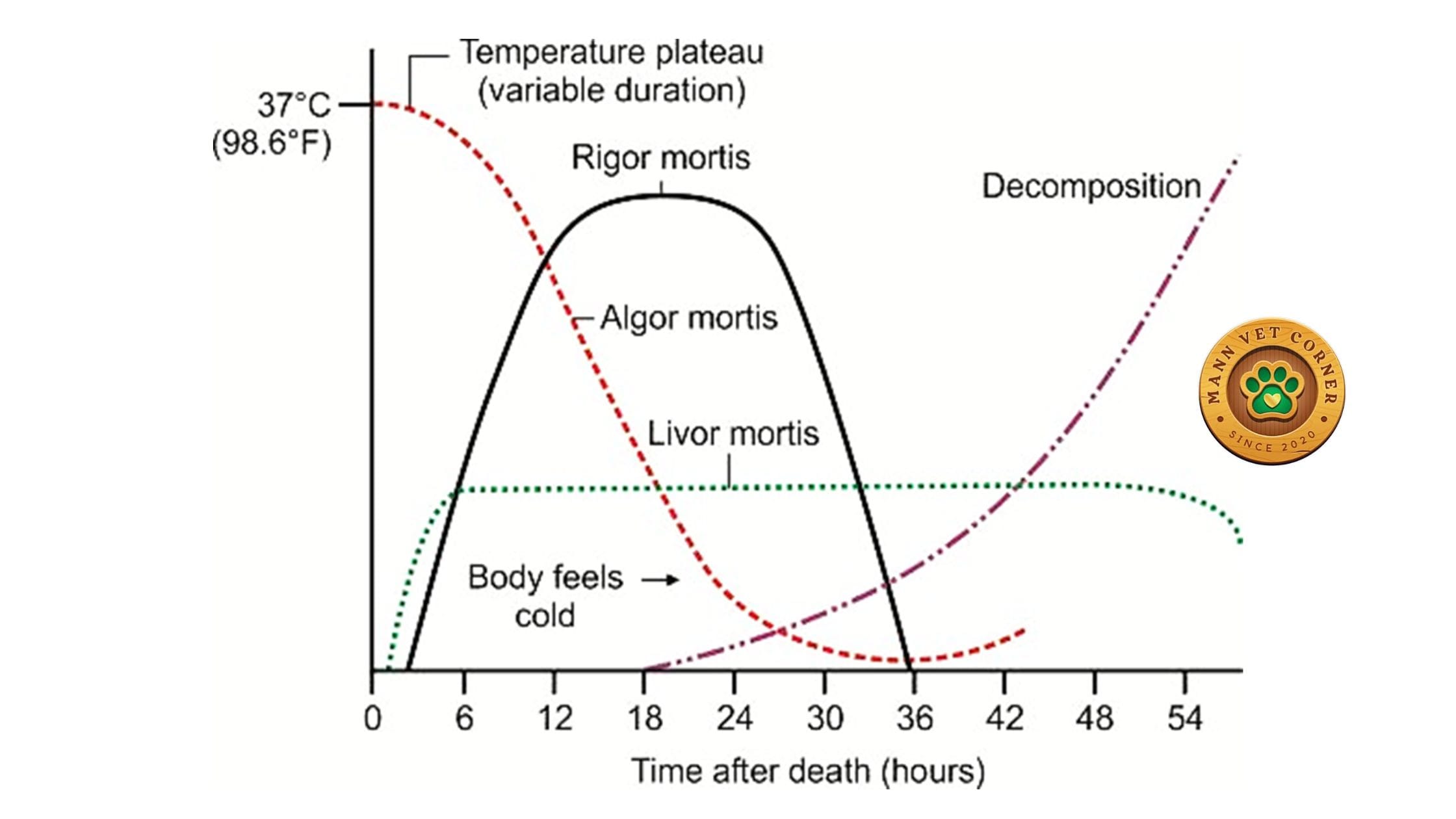
Algor mortis is the gradual cooling of the body toward ambient environmental temperature after death. Once circulation ceases, the body can no longer generate or regulate heat, and heat dissipates through conduction, convection, and radiation.
Timeline and Pattern
- During the first 1–5 hours, body temperature may remain relatively stable (the “temperature plateau”)
- Cooling is fastest during the first few hours then gradually slows as the temperature differential between body and environment narrows
- Algor mortis is only reliably useful as a PM indicator within the first 24 hours after death
The Rule of Thumb
As a general guideline for estimating time of death using body temperature:
- The body loses approximately 1.5–2°F per hour during the first 12 hours
- This slows to approximately 1°F per hour for the next 12–18 hours
Practical Calculation Example
If a body temperature of 95.4°F is recorded at 7:25 AM, and normal body temperature is 98.4°F:
(98.4 – 95.4) ÷ 1.5 = 2 hours since death 7:25 AM – 2 hours = Approximate time of death: 5:25 AM
Factors That Modify Algor Mortis
Algor mortis must always be interpreted in context. The following factors affect how quickly or slowly the body cools: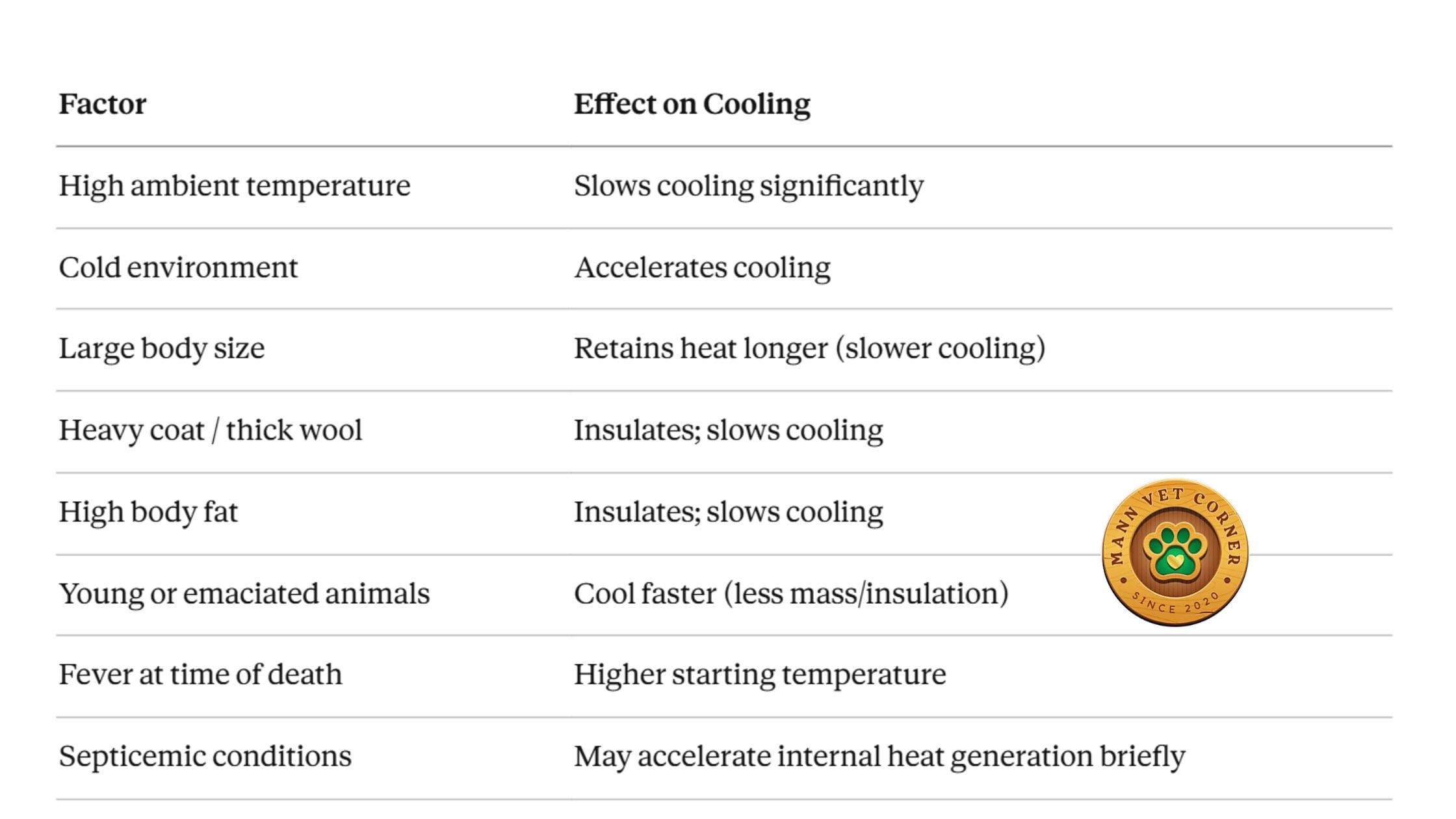 Clinical Note: Always record the ambient temperature, species, body condition score, and coat density alongside your temperature measurement. Algor mortis alone is never definitive — it is one tool in a broader picture.
Clinical Note: Always record the ambient temperature, species, body condition score, and coat density alongside your temperature measurement. Algor mortis alone is never definitive — it is one tool in a broader picture.
3. Rigor Mortis — Postmortem Muscle Stiffening
Rigor mortis is the temporary stiffening of skeletal and cardiac muscle following death. It is one of the most practically useful early postmortem signs and provides important clues about time of death and postmortem handling of the carcass.
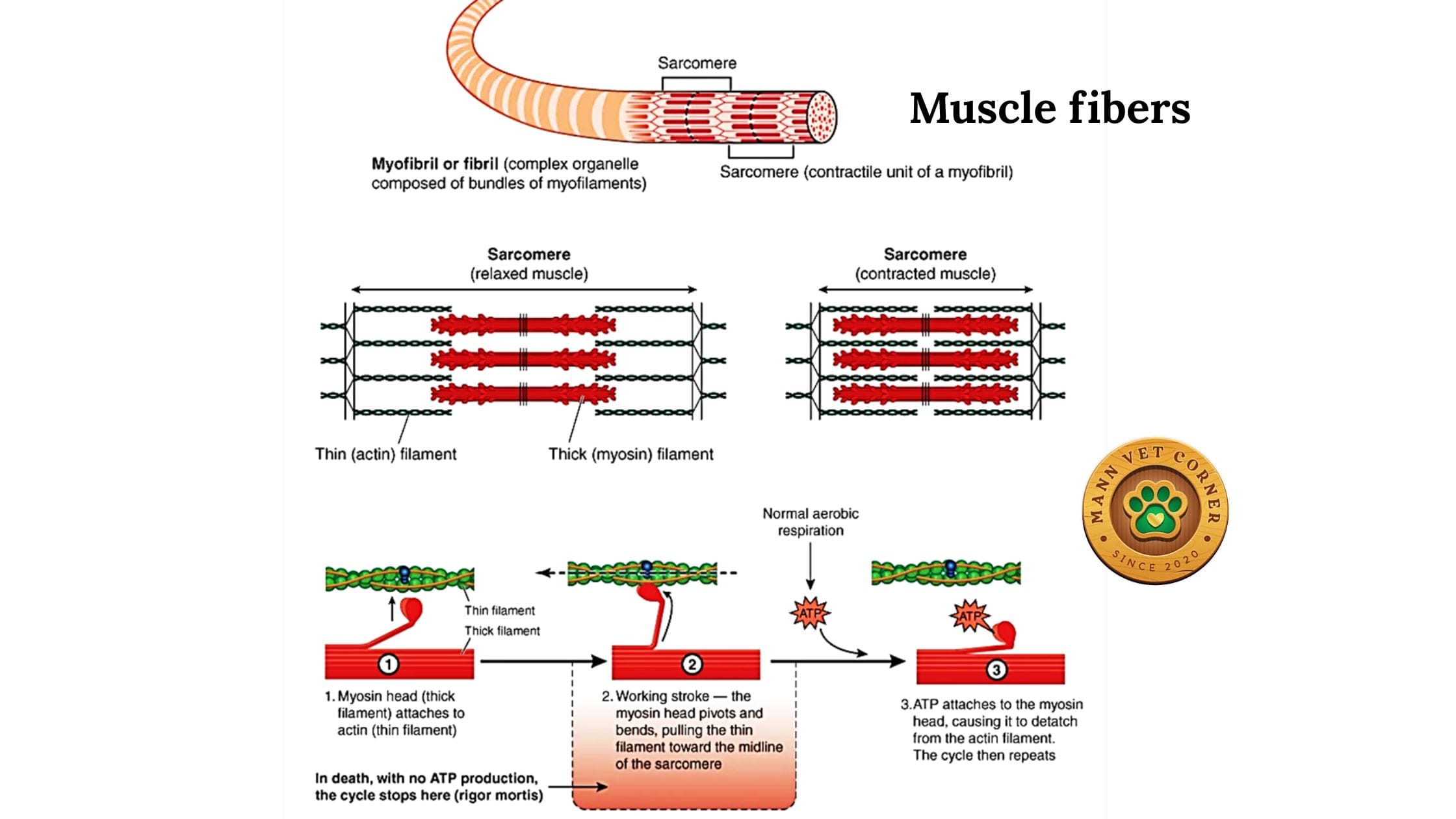
The Biochemical Mechanism
Understanding why rigor mortis occurs helps you interpret it correctly:
- At death, muscle cells enter anoxia — oxygen supply ceases
- ATP synthesis drops dramatically; the cell switches to anaerobic glycolysis
- Glycogen stores are rapidly depleted, producing pyruvic acid and lactic acid
- These metabolic byproducts accumulate intracellularly (no circulation to remove them)
- Intracellular pH falls from 7.0 to approximately 5.6
- The drop in pH, combined with declining ATP and rising free calcium, locks myosin heads to actin filaments
- Without ATP to break this bond, muscles remain in a state of permanent contraction
As putrefaction proceeds and proteolytic enzymes begin breaking down muscle proteins, rigor eventually resolves on its own.
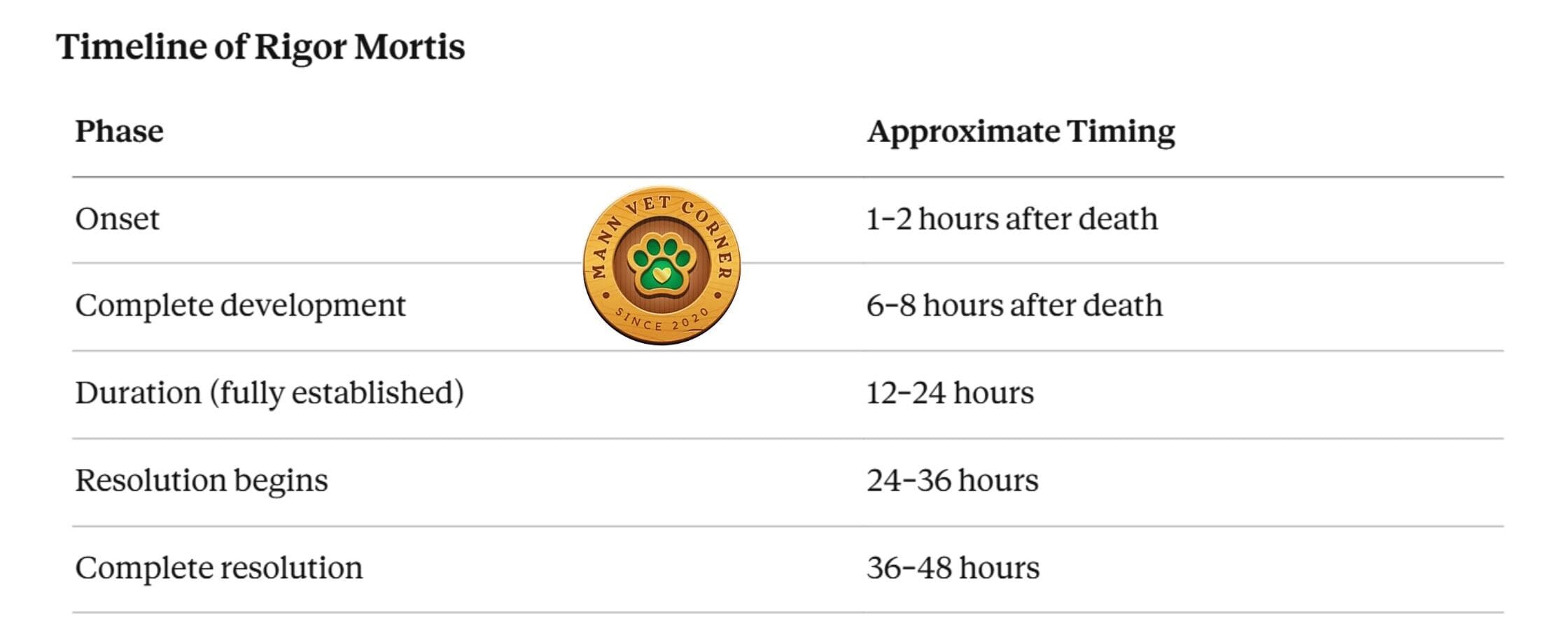
Timeline of Rigor Mortis
Rigor mortis develops and resolves in a characteristic head-to-tail pattern:
- Jaw and facial muscles — stiffen first (important to check at initial examination)
- Neck and forelimbs — stiffen next
- Hindlimbs and trunk muscles — affected last
Resolution follows the same sequence in reverse — jaw muscles soften first, hindlimbs last.
Assessing Rigor at Necropsy
Before beginning any necropsy, always assess and document the degree of rigor mortis:
- Complete rigor: All muscle groups stiff; joints resist passive movement
- Partial rigor: Some muscle groups affected; others relaxed
- Absent rigor: Muscles are flaccid (very early or late postmortem)
 Factors That Modify Rigor Mortis
Factors That Modify Rigor Mortis
Species:
- Birds and small mammals: rapid onset and resolution
- Large animals (cattle, horses): slower onset and longer duration
Age and body condition:
- Young, old, or malnourished animals may show weak or incomplete rigor due to reduced muscle glycogen and mass
Cause of death:
- Sudden violent death or acute poisoning → very rapid onset (muscles are glycogen-rich)
- Chronic wasting disease or starvation → delayed or weak rigor (glycogen depleted antemortem)
- Clostridial diseases (e.g., tetanus) → premature stiffness from toxin-induced muscle spasms
Temperature:
- Warm climates (>20°C): onset within hours, resolves within ~12 hours
- Cold climates (<10°C): rigor onset is delayed and may be incomplete or absent
Special situations:
- Drowning victims may show delayed rigor due to prolonged hypoxia
- Septicemic animals may show accelerated rigor due to tissue acidosis
Forensic Value of Rigor Mortis
Rigor mortis also reveals whether a carcass has been moved after death. If rigor has set in a particular position but the body is now found in a different position, this is significant evidence of postmortem repositioning.
4. Livor Mortis (Hypostasis) — Postmortem Blood Pooling
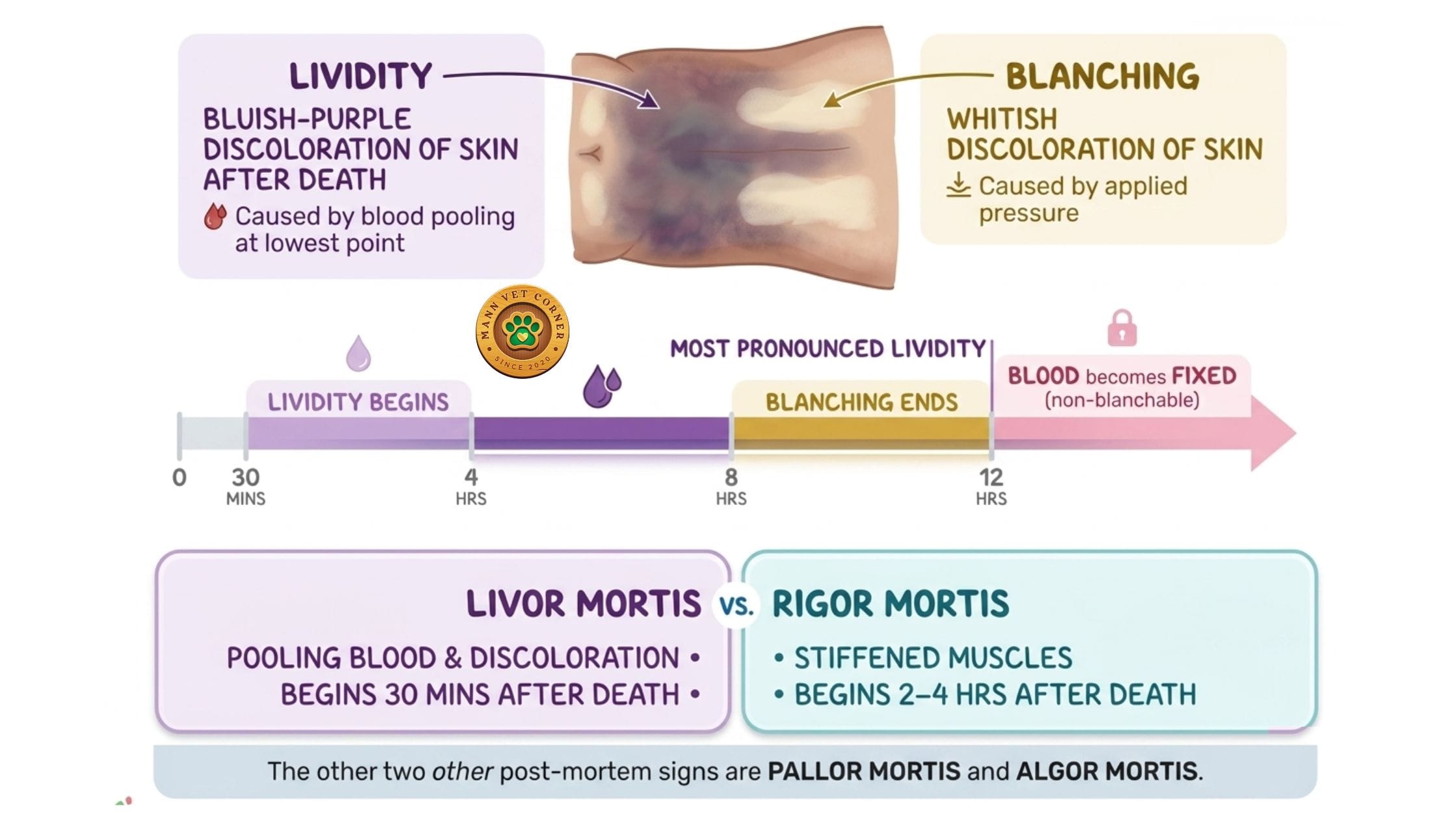
Livor mortis, also known as hypostasis or cadaveric lividity, is the gravitational settling of blood into the lower, dependent portions of the body after circulation ceases.
What It Looks Like
- Blood pools in the lowest parts of the body, causing a characteristic purplish-red discoloration of the skin and internal tissues
- Areas in contact with firm surfaces (ground, walls) remain pale due to compression of blood vessels — creating a “negative imprint” of whatever the body was resting on
- As putrefaction begins, these areas change color: first green (due to sulphohemoglobin formation), then brown-black
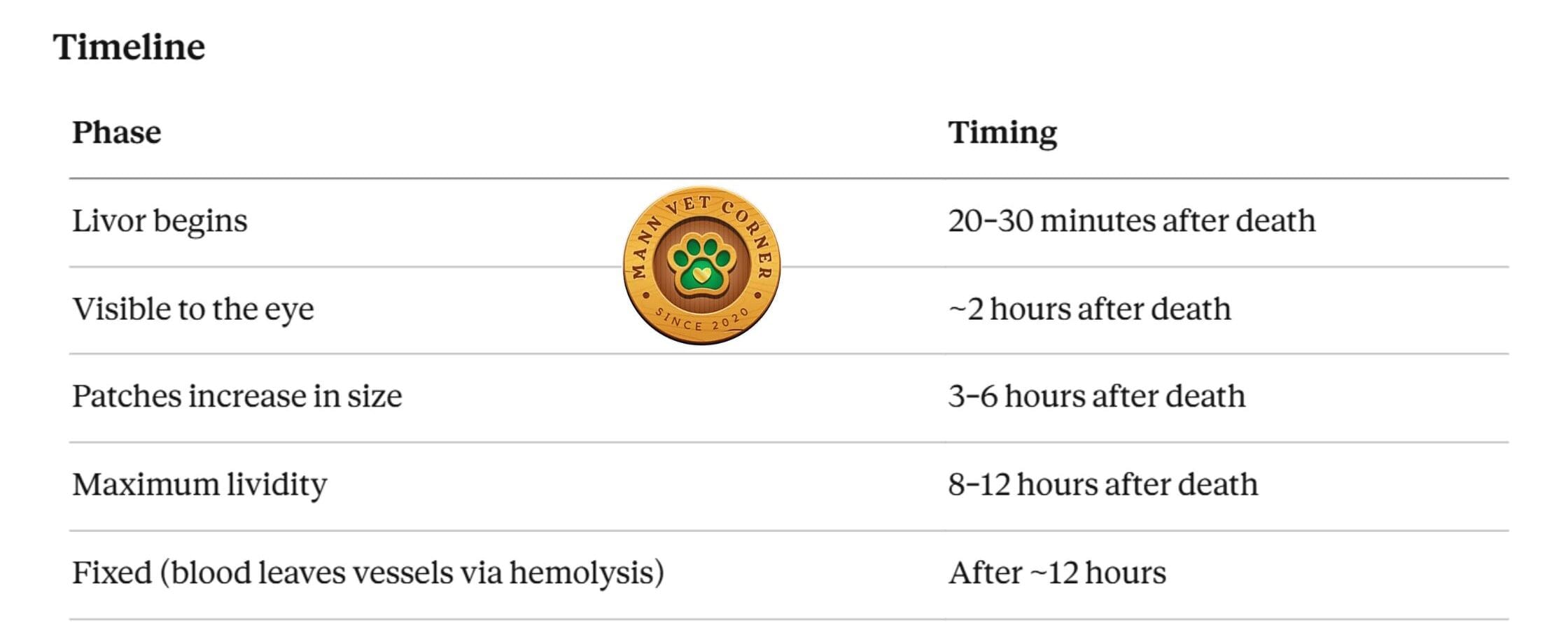
Initially, livor mortis is moveable — if the body is repositioned within the first 6–8 hours, blood will shift to the new dependent areas. After approximately 12 hours, hemolysis causes red blood cells to rupture and hemoglobin to diffuse into surrounding tissues. Once this occurs, livor mortis becomes fixed and will not shift even if the body is moved.
Forensic Significance
This fixation property makes livor mortis one of the most valuable forensic tools available:
- Confirming body position at time of death: If the pattern of lividity is inconsistent with how the body is currently positioned, the body was moved after death
- Determining whether the carcass was dragged or relocated: Patterns of pressure pallor reveal contact objects
- Estimating time of death in combination with other findings
5. Postmortem Emphysema
Postmortem emphysema refers to the accumulation of gas in body cavities, tissues, and solid organs as a result of bacterial fermentation — primarily by anaerobic organisms from the gastrointestinal tract.
Gases produced include:
- Methane
- Carbon dioxide
- Ammonia
- Hydrogen sulfide
These gases collectively generate the characteristic odor of putrefaction.
Secondary effects of gas accumulation:
- Distension of abdominal and thoracic cavities
- Emphysematous appearance of parenchymal organs (liver, spleen appear spongy)
- Rupture of hollow organs due to internal pressure and wall weakening from putrefaction
- Displacement of organs, particularly intestines
Critical Distinction: Always differentiate postmortem gas accumulation from antemortem bloat (e.g., ruminal tympany, intestinal obstruction). Antemortem bloat typically shows other signs of pre-death distress and may have associated lesions. Postmortem emphysema is usually more diffuse and involves multiple compartments.
6. Postmortem Imbibition
Imbibition refers to the displacement or diffusion of fluids into surrounding tissues after death. Two important types occur:
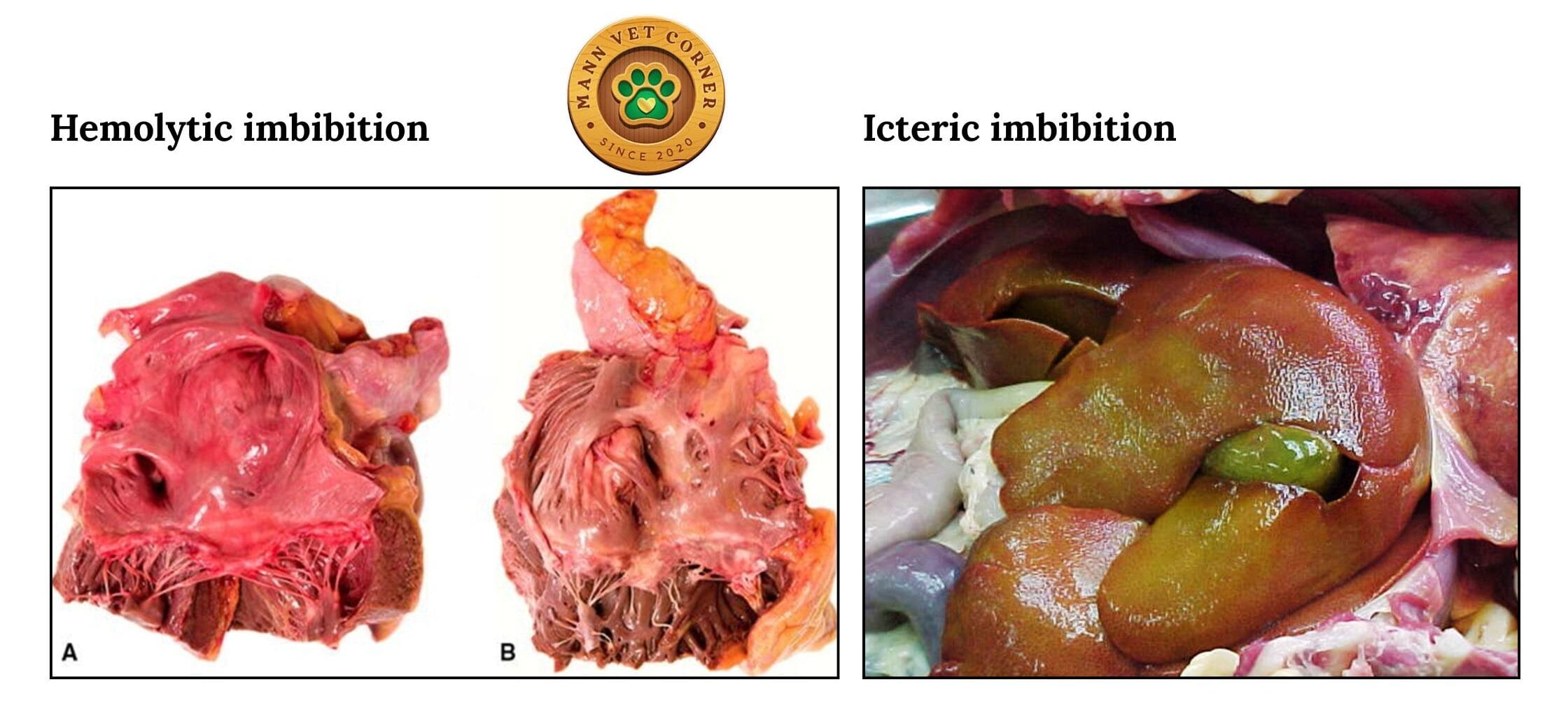
Hemolytic Imbibition
After death, red blood cells undergo intravascular hemolysis — the cell membranes break down, releasing hemoglobin into plasma. This free hemoglobin then diffuses through blood vessel walls and permeates surrounding tissues.
- Appearance: Uniform reddish discoloration of tissues that darkens over time as hemoglobin oxidizes
- Distribution: Generalized throughout the carcass; tends to increase during the necropsy as tissues are disturbed
- Key distinction from antemortem hemorrhage: Hemolytic imbibition produces uniform discoloration without the focal or patchy distribution typical of true hemorrhage.
Icteric Imbibition
Bile and bile pigments diffuse through the walls of the gallbladder into adjacent organs — particularly the liver and nearby intestinal serosa.
- Appearance: Well-defined yellow-green discoloration of liver tissue and adjacent structures
- Important: This must be differentiated from true icterus (jaundice), which is an antemortem condition caused by elevated bilirubin. True icterus discolors tissues systemically and uniformly; icteric imbibition is localized to gallbladder contact areas.
Part 4: Late Postmortem Changes
5. Decomposition
Decomposition is the comprehensive postmortem breakdown of a carcass, driven by two simultaneous processes:
Autolysis: The self-digestion of tissues by the body’s own intracellular enzymes (mainly lysosomal hydrolases), released when cells lose membrane integrity under anoxic conditions.
Putrefaction: The breakdown of tissues by bacteria — initially the body’s own commensal organisms from the respiratory and digestive tracts, later augmented by environmental microorganisms.
Both processes release chemical compounds including cadaverine and putrescine — the diamines primarily responsible for the characteristic odor of a decomposing carcass.
Autolysis in Detail
Autolysis is the first process to begin, even before bacteria have extensively colonized dead tissue. It is accelerated by:
- High temperature (heat dramatically speeds enzyme activity)
- Tissues with high enzyme content — pancreas, liver, kidney, adrenal medulla, and intestinal mucosa are first affected
- Tissues with low enzyme content — bone, cartilage, connective tissue, and skeletal muscle are more resistant
Distinguishing autolysis from antemortem lesions:
Grossly:
- Autolytic tissue is uniformly pale or uniformly discolored — not focal
- Autolytic organs are fragile and rupture easily under minimal pressure
- Autolytic intestines may rupture during handling — always a sign of advanced autolysis, not necessarily an antemortem lesion
Microscopically:
- Antemortem necrosis shows focal or patchy distribution, hyperemia, and surrounding inflammatory infiltrate
- Autolysis shows uniform loss of nuclear and cytoplasmic detail, intravascular erythrocyte lysis, and absence of inflammatory reaction
Stages of Decomposition
Decomposition progresses through five recognizable stages, each with characteristic features:
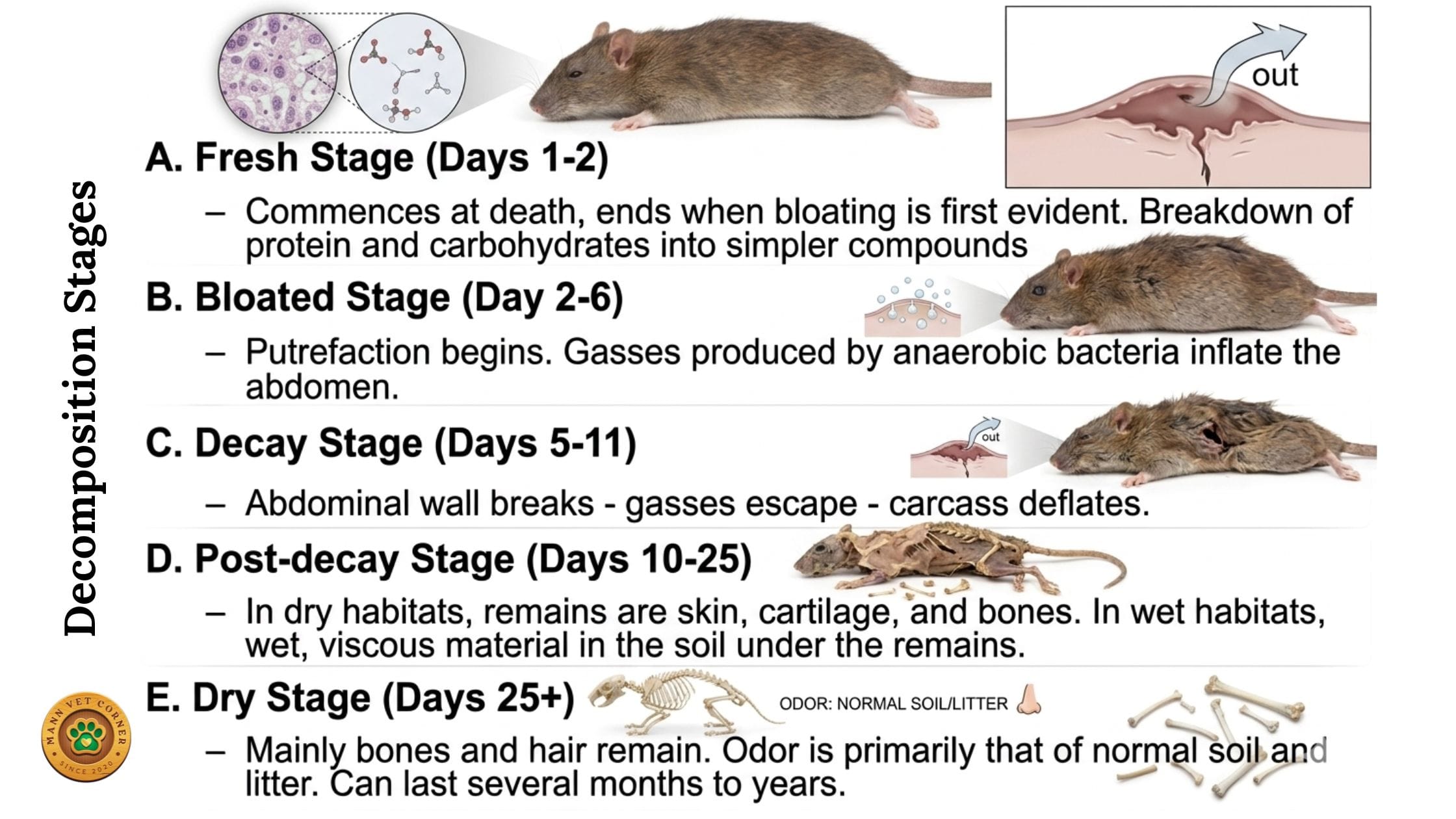
A: Fresh (Days 1–2)
- Commences at the moment of death
- Ends when bloating becomes evident
- Proteins and carbohydrates begin breaking down into simpler compounds
- Blowflies arrive and deposit eggs around the eyes, nostrils, mouth, and genitoanal openings
- Essentially appears as a recently deceased animal with primary relaxation
B: Bloated (Days 2–6)
- Putrefaction begins in earnest
- Anaerobic bacteria produce gases that distend the abdomen
- Cadaver begins to swell and emit strong odor
- Blowflies continue laying eggs; flesh flies appear
- Small maggots begin feeding on exposed tissues
C: Decay (Days 5–11)
- Abdominal wall may rupture; gases escape and the carcass deflates
- Large masses of maggots feed both externally and internally
- Adult blowflies are no longer attracted; predators and parasitoids of maggots arrive
D: Post-Decay (Days 10–25)
- Cadaver is drying out; large maggots leave to pupate
- In dry habitats: skin, cartilage, and bone remain
- In wet habitats: viscous material remains in soil under the carcass
E: Dry (Days 25+)
- Mainly bones, some dried skin and hair remain
- Insects capable of digesting keratin (clothes moths, mites, dermestid beetles) are active
- Odor resembles normal soil; stage can last months to years until skeletonization is complete
Important: The duration of each stage is heavily influenced by season and temperature. Summer decomposition may complete in weeks; winter decomposition at the same site may take months. This has direct implications for estimating time of death in cases found outdoors.
6. Putrefaction
Putrefaction is the specifically bacterially-driven component of decomposition, involving enzymatic degradation of all organic matter by bacteria, fungi, and arthropods.
The process is carried out by:
- Aerobic commensals of the respiratory and GI tracts (early)
- External bacteria that invade dead tissues
- Eventually dominated by anaerobic microorganisms as oxygen depletes
Putrefaction results in a rapid drop in pH, which ironically accelerates the growth of anaerobic fermenters located primarily in the gastrointestinal tract — creating a self-reinforcing cycle of decomposition.
The green discoloration seen in abdominal organs early in putrefaction results from the formation of sulphohemoglobin, as hydrogen sulfide gas reacts with hemoglobin in pooled blood.
7. Mummification
Mummification is an alternative decomposition pathway that occurs when a carcass is placed in an environment that is hot, dry, and well-ventilated. Rather than liquefying, tissues lose moisture faster than bacteria can proliferate, resulting in desiccation of the carcass.
Characteristics of mummified remains:
- Skin becomes dark, dry, and leathery
- Body is significantly reduced in size and weight
- Tissues are preserved in a desiccated but structurally intact state
- Bacterial decomposition is greatly reduced
Mummification is relatively common in arid climates, in sheltered outdoor locations with low humidity, or in stillborn/neonatal animals in dry environments. Internally, mummified fetuses may be retained within the uterus of livestock.
8. Skeletonization
Skeletonization represents the final stage of decomposition — the complete elimination of all soft tissue, leaving only disarticulated bones.
- Soft tissue remnants dry and fall away
- Bones may be bleached by sunlight and weather (surface bone)
- Ligaments and cartilage are the last soft structures to remain
- The timeline from death to skeletonization can range from weeks (in tropical environments with abundant scavengers) to years (in cold or arid environments)
At this stage, the only information recoverable is skeletal — species identification, age estimation, sex determination, and evidence of antemortem bony lesions or trauma.
Part 5: A Practical Field Decision Guide
When you approach a dead animal, use the following systematic approach to assess postmortem stage and estimate time of death:
1st step: External Assessment Before Touching the Carcass
- Note the position of the body
- Look for obvious signs of lividity (dependent discoloration)
- Note presence or absence of bloating or gas distension
- Note insect activity (blowfly eggs, maggots, stage of maggot development)
- Assess coat/skin dryness and corneal opacity
- Smell (absence of odor = very early; mild odor = putrefaction beginning; strong odor = decay stage)
2nd step: Assess Rigor Mortis
- Gently attempt to move the jaw, neck, and forelimbs
- Classify as: absent / partial / complete / resolving
- Correlate with ambient temperature
3rd step: Measure Body Temperature
- Record rectal temperature with a thermometer
- Record ambient temperature
- Apply the cooling formula to estimate hours since death
- Remember this is only reliable within the first 24 hours
4th step: Assess Livor Mortis
- Observe pattern of gravitational discoloration
- Is it consistent with the current body position?
- Is it fixed or movable? (Press on an area — does it blanch?)
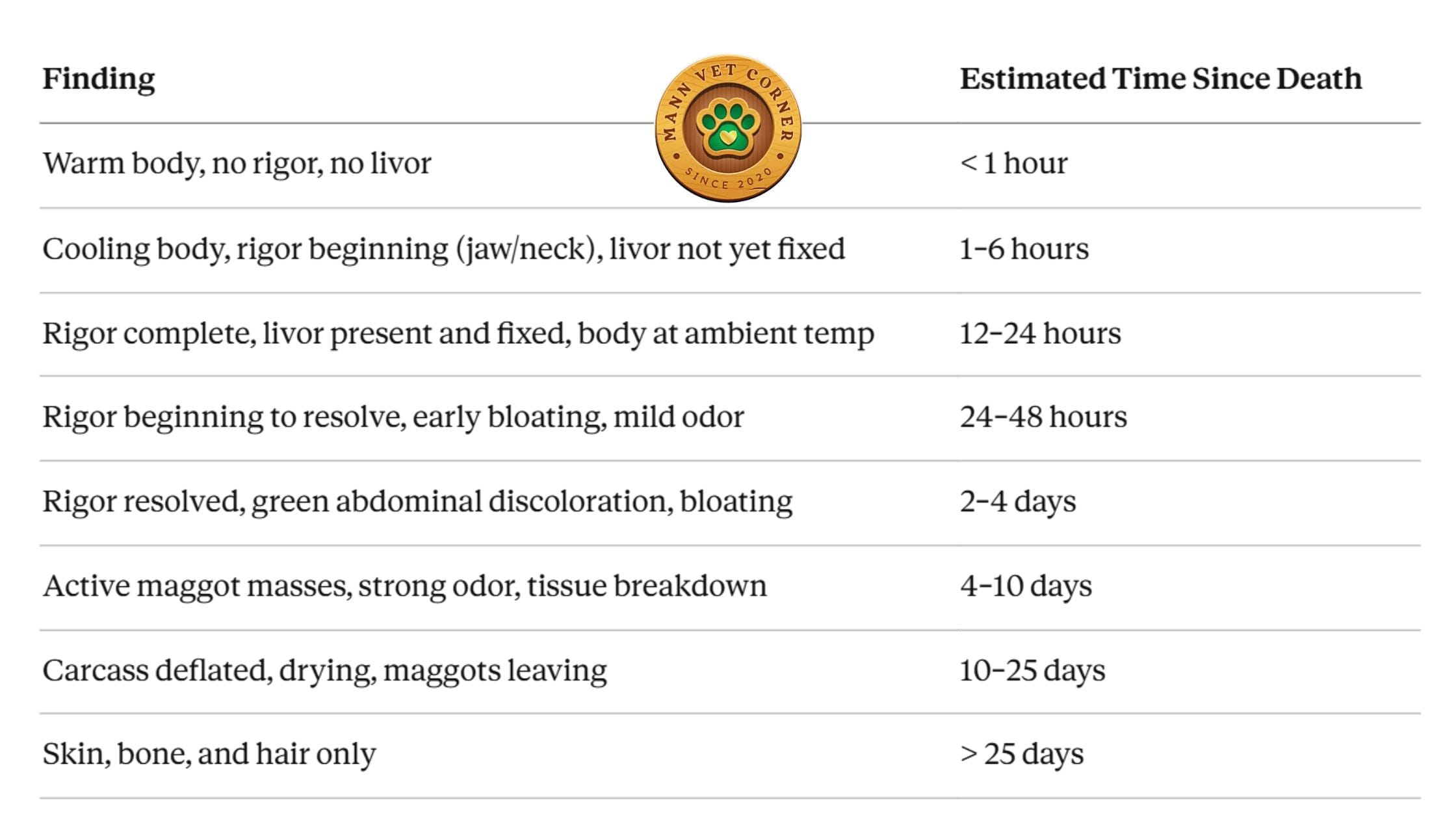
5th step: Integrate All Findings
Use the table below to synthesize your observations:
Part 6: Key Pitfalls and Common Errors
1. Confusing postmortem emphysema with antemortem bloat Look for other signs of pre-death distress. Antemortem bloat in ruminants causes ante-mortem signs and the rumen will be affected specifically.
2. Misidentifying hemolytic imbibition as hemorrhage True hemorrhage is focal, has defined margins, and may show fibrin, clot, or surrounding tissue reaction. Hemolytic imbibition is diffuse, uniform, and deepens as you work.
3. Mistaking autolytic intestinal rupture for an antemortem perforation Autolytic intestines rupture with minimal force and show no inflammatory reaction at the edges. Antemortem perforations show fibrinous peritonitis and reactive changes.
4. Over-relying on a single PM indicator for time of death Always triangulate — use rigor, livor, algor mortis, dehydration, insect activity, and environmental conditions together. No single sign is reliable in isolation.
5. Failing to note the position of lividity before moving the carcass Once the body is moved for necropsy, you lose the opportunity to assess whether the livor pattern matches the death position. Always document this first.
Conclusion
Postmortem changes are not simply the decay of a dead animal — they are a biological record of the time, conditions, and circumstances of death. For a veterinarian performing a necropsy, reading these changes accurately is as important as interpreting the internal lesions you will find.
By systematically assessing cadaver dehydration, algor mortis, rigor mortis, livor mortis, emphysema, imbibition, and the stage of decomposition — and by integrating these findings with species, body condition, environment, and history — you can arrive at a well-reasoned estimate of time of death and an accurate interpretation of what is truly pathological versus what is artifact.
This skill is essential not only for routine diagnostic necropsies, but also for medicolegal investigations, insurance claims, welfare cases, and disease outbreak investigations where the timing and circumstances of animal deaths are critical evidence.
This article is intended for veterinary professionals and veterinary students. All timelines and values given are approximations and should be interpreted in clinical context. Environmental variables significantly affect all postmortem processes.